Q&A with Professor Warren Rozen: Dupuytren’s Disease
Q1. Tell us about the condition of Dupuytren’s contracture. What is it and how does it affect function?
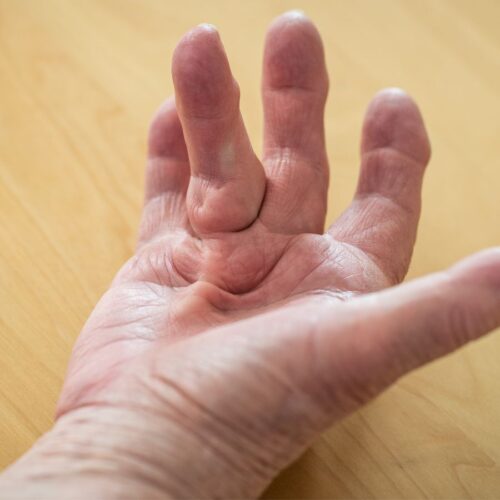
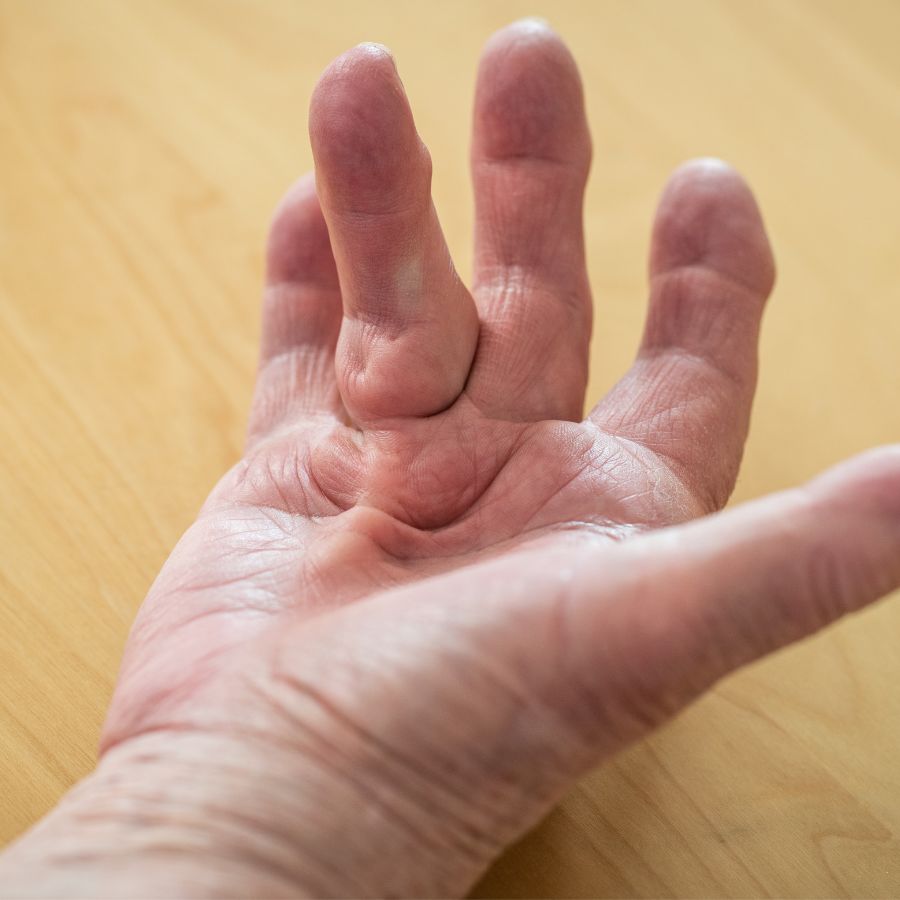
Dupuytren’s disease or Dupuytren’s ‘contracture’ is a common condition that affects the hand and fingers, specifically affecting the connective tissue beneath the skin of the palm. It is characterised by the thickening and tightening of this tissue, forming nodules or cords that can cause the fingers to shift into a bent position.
As the disease progresses, affected fingers may become permanently bent, which can lead to functional problems, such as difficulty in performing tasks like grasping objects or shaking hands. The severity of Dupuytren’s contracture varies, with some experiencing mild disease and others having more severe deformities.
We don’t know what causes Dupuytren’s contracture but there is likely to be a genetic component as it tends to run in families. More common among men over 50, and in people of Northern European descent, leading to its nickname ‘Viking’s disease’.
Q2. Professor Rozen, you have published widely about collagenase injection for Dupuytren’s. How does this work and how does it differ from other methods of treatment? How effective and safe is it?
Collagenase is an enzyme that works by breaking down the collagen fibres that form the thickened cords in the palm, allowing the fingers to straighten.
Instead of cutting out the contracted tissue, collagenase is injected directly into the affected area. The enzyme then weakens and breaks down the collagen, making it easier to manipulate and straighten the fingers.
The effectiveness of collagenase treatment varies depends on the severity of the contracture and some individual factors. Our research studies have shown that collagenase injections can improve finger extension in many patients, often achieving complete straightening of the affected fingers. It’s important to note that there is a rate of recurrence ranging from 20% to 50% within 5 years after treatment, but this can be the case with surgery too.
Collagenase injections for Dupuytren’s contracture are considered safe and well-tolerated. As with any medical procedure, there are potential risks and side effects, including swelling, bruising, and pain at the injection site. Some patients may also experience temporary numbness in the fingers. There is a small risk of more serious complications, such as tendon rupture or nerve injury, but these are rare.
Q3. What is the procedure for manipulation after injection? What can be done to minimise complications?
After the injection of collagenase, the procedure for manipulation involves a manual straightening of the affected finger(s) within 1-7 days. This manipulation is performed to break the weakened collagen fibres and improve finger extension. During the manipulation, pressure and gentle stretch is applied to the finger(s) for straightening. This is usually performed under local anaesthesia or nerve blocks.
There are potential complications associated with the manipulation procedure. One possible complication is skin tears which can occur more frequently if the skin is fragile or in cases of more severe contracture.
These risks are minimised by careful injection and manipulation techniques, clinician expertise and experience. Close postoperative care including hand therapy, intermittent immobilization, splinting and wound/swelling management as needed.
Q4. What are the long-term follow-up results for patients who have had collagenase injection for Dupuytren’s?
There is now really good data looking at long-term follow-up for patients who have had collagenase injection for Dupuytren’s contracture, and these largely show extremely positive outcomes. Studies generally report that collagenase injection effectively reduces contracture and improves hand function in the majority of patients. We are really proud that Australia has been at the forefront of much of this research.
Q5. Collagenase injection sounds like an effective treatment but it doesn’t seem to commonly performed in public hospitals. Why is this the case?
Until recently, Collagenase was being used quite broadly in both public and private sectors in Australia. This was occurring at a rapidly increasing rate as good data on its use was more widespread as experience grew. However, the cost of the drug increased several years ago, and its listing on the PBS in Australia lapsed, which meant the procedure is no longer rebatable under Medicare. Research demonstrating the cost advantages of Collagenase injection over surgery will help current advocacy efforts in having this drug re-listed on the PBS, so that it can benefit more patients in the future.
Learn more about Professor Rozen’s research here, or to find his contact details follow the link to our find a surgeon page.
Featured Stories

Member Blog with Dr Ellis Choy: What is a Deep Plane Facelift?
Who is the ideal candidate for a deep plane facelift?…
Continue reading Like
Like

