Procedures
Sclerotherapy (treatment of spider veins)
- About Your Specialist Plastic Surgeon
- Cosmetic
- Non-surgical Procedures
- Plastic Surgery Glossary
- Questions for Your Surgeon
- Reconstructive
- Surgical Procedures
- Abdominoplasty (cosmetic)
- Abdominoplasty (muscle repair postpartum)
- Arm Lift
- Body Contouring
- Body Lift
- Breast Asymmetry Correction
- Breast Augmentation (implants)
- Breast Implants with Lift
- Breast Lift
- Breast Reconstruction
- Breast Reduction
- Brow Lift
- Burns and Scarring
- Chest Surgery
- Chin Surgery
- Cleft Lip & Palate
- Ear Surgery
- Eyelid Reduction Surgery
- Facelift Surgery
- Facial Implants
- Facial Procedures
- Fat Injection
- Genital Reconfiguration Surgery
- Gluteal Augmentation or Buttocks Lift
- Gynaecomastia (male breast reduction)
- Hair Replacement Surgery
- Hand Surgery
- Labiaplasty
- Liposuction
- Lymphoedema Surgery
- Nipple Enhancement for Inverted Nipples
- Nose Surgery
- Scar Revision
- Skin Cancer
- Thigh Lift
- Tissue Expansion
- Voice Surgery
Sclerotherapy (treatment of spider veins)
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
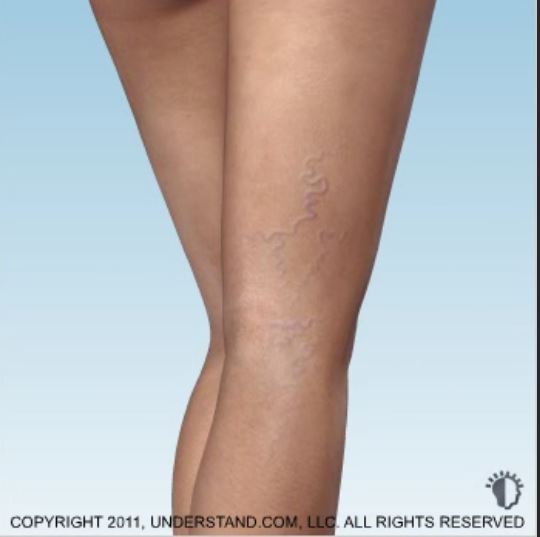
Sclerotherapy is the treatment of small yet unsightly clusters of red, blue or purple veins that most commonly appear on the thighs, calves and ankles. These veins are also known as “spider veins”.
Sclerotherapy treats spider veins by injecting sclerosing solution into affected veins. This causes the veins to collapse and fade from view. The procedure may also remedy bothersome symptoms associated with spider veins, including aching, burning, swelling and night cramps.
Sclerotherapy is a highly individualised procedure and may not be suitable for everyone. Always talk to your Specialist Plastic Surgeon before making a decision. Your surgeon will assess your condition and general health, and plan the treatment that is best suited to you.
Before you decide to undergo sclerotherapy, there are some important issues to keep in mind:
- If you are pregnant or breastfeeding, you may be advised to postpone sclerotherapy treatment. In most cases, spider veins that surface during pregnancy will disappear on their own within three months after the baby is born. Also, because it is not known how sclerosing solutions may affect breast milk, nursing mothers are usually advised to wait until after they have stopped breastfeeding
- If more serious “deep vein” problems are detected, your surgeon may refer you to a different specialist for further evaluation. Problems with the larger veins must be treated first, or sclerotherapy of the surface veins will be unsuccessful
- Not every affected vein will disappear after treatment, you need to have realistic expectations of the procedure
- The procedure will only treat veins that are currently visible. It cannot prevent new veins from surfacing in the future
- Individuals with hepatitis, AIDS or other blood-borne diseases may not be candidates for sclerotherapy. Patients with circulatory problems, heart conditions, or diabetes may also be advised against treatment
Sclerotherapy may be a good option for you if:
- You are physically healthy
- You have realistic expectations
Sclerotherapy does not require anaesthesia.
Sclerotherapy is generally safe but does have the potential for risks and complications to occur.
Some risks and complications associated with sclerotherapy may include but are not limited to:
- Formation of blood clots in the veins
- Severe inflammation
- Adverse allergic reactions to the sclerosing solution
- Skin injury that could leave a small but permanent scar
- Pigmentation irregularity including brownish splotches on the affected skin that may take months to fade, sometimes up to a year
- The appearance of fine reddish blood vessels around the treated area known as “telangiectatic matting”. Further injections may be required
Sclerotherapy is usually performed as a day case in an accredited day surgery.
Before undergoing the procedure, it is important that you:
- Be as fit as possible to help the recovery process
- Stop smoking
- Do not apply any type of moisturiser, sun block or oil to your legs on the day of your procedure
Your Specialist Plastic Surgeon will also examine you for signs of more serious “deep vein” problems, often indicated by swelling, sores, or skin changes at the ankle. A hand-held Doppler ultrasound device is sometimes used to detect any backflow within the venous system. If such problems are identified, your surgeon may refer you to a different specialist for further evaluation. Problems with the larger veins must be treated first, or sclerotherapy of the surface veins will be unsuccessful.
Your doctor will ask you about any other problems you may have with your legs, such as pain, aching, itching or tenderness. You will also be asked about your medical history, medications you take, or conditions that would preclude you from having treatment.
Your surgeon should give detailed instructions to prepare for the procedure. Follow them carefully.
After the procedure, compression tape will be applied both during and after the procedure. Tight-fitting support hose may also be prescribed to guard against blood clots and to promote healing.
It is normal to experience some cramping in the legs for the first day or two after the injections. This temporary problem usually doesn’t require medication.
You will be encouraged to walk to prevent clots from forming in the deep veins of the legs. Prolonged sitting and standing should be avoided, as should squatting, heavy weight lifting and “pounding” type exercises, including jogging.
Your treated veins will look worse before they begin to look better. You will notice bruising and reddish areas at the injection sites once the compression dressings are removed. The bruises should diminish within one month. Sometimes, there may be residual brownish pigmentation which may take up to a year to completely fade.
Your surgeon will give you specific instructions on post-procedural care. Be sure to follow them carefully.
Depending on the extent of the problem, further treatment may be necessary to achieve the optimal result. A second series of injections are sometimes necessary in severe cases.
Cost is always a consideration in elective procedures. Prices for individual procedures can vary widely between Specialist Plastic Surgeons. Some factors that may influence the cost include the surgeon’s experience, the type of procedure used and the geographic location of the office.
Costs associated with the procedure may include:
- Surgeon’s fee
- Hospital or surgical facility costs
- Anaesthesia fees
- Prescriptions for medication
- Medical tests
Your surgeon should welcome any questions you may have regarding fees.
Sclerotherapy:
The treatment of small yet unsightly clusters of red, blue or purple veins through the injection of sclerosing solution into affected veins
Telangiectatic matting:
The appearance of fine reddish blood vessels around the treated area
Visit the Plastic Surgery Glossary for more medical terms.
This website is intended to provide you with general information only. This information is not a substitute for advice from your Specialist Plastic Surgeon and does not contain all the known facts about this procedure or every possible side effect of surgery. It is important that you speak to your surgeon before deciding to undergo surgery. If you are not sure about the benefits, risks and limitations of treatment, or anything else relating to your procedure, ask your surgeon to explain. Patient information provided as part of this website is evidence-based, and sourced from a range of reputable information providers including the American Society of Plastic Surgeons, Better Health Channel and Mi-tec medical publishing.
Featured Stories

ASPS welcomes new Ahpra guidelines for Non-Surgical Cosmetic Practitioners
Sydney. June 3, 2025: The Australian Society of Plastic Surgeons…
Continue reading